1. Introduction
Tracheal bronchus or pig bronchus is a rare congenital anomaly where an ectopic bronchus arises from the lateral wall of the trachea, more commonly from the right side (1), above the carina and ventilates the upper lobe. Tracheal bronchus is usually asymptomatic, however in some patients it is presented with recurrent pneumonia and atelectasis (2-4). It can be associated with Down syndrome, congenital heart diseases and costovertebral anomalies (5-7). The current study reported a five months old infant with history of recurrent pneumonia diagnosed with tracheal bronchus in conjunction with unilateral (right) absence of pulmonary artery (UAPA). To the authors’ best knowledge, this association was a very rare condition.
2. Case Presentation
The patient was a five-month-old infant referred to the clinic with chief complaint of coughing, rapid breathing and wheezing from one month ago, which had led to three times hospitalization in another health care center during the time and because of poor response to treatment, she was referred to the pediatric infectious disease clinic.
On physical examination, she looked around consciously. She was febrile (rectal 38°C); her respiratory rate was 55 per minute and blood oxygen saturation was 92%. She had course crackles in her lungs auscultation and subcostal retraction was obvious. Other physical examinations were normal. She was admitted to the current study our hospital for further examination.
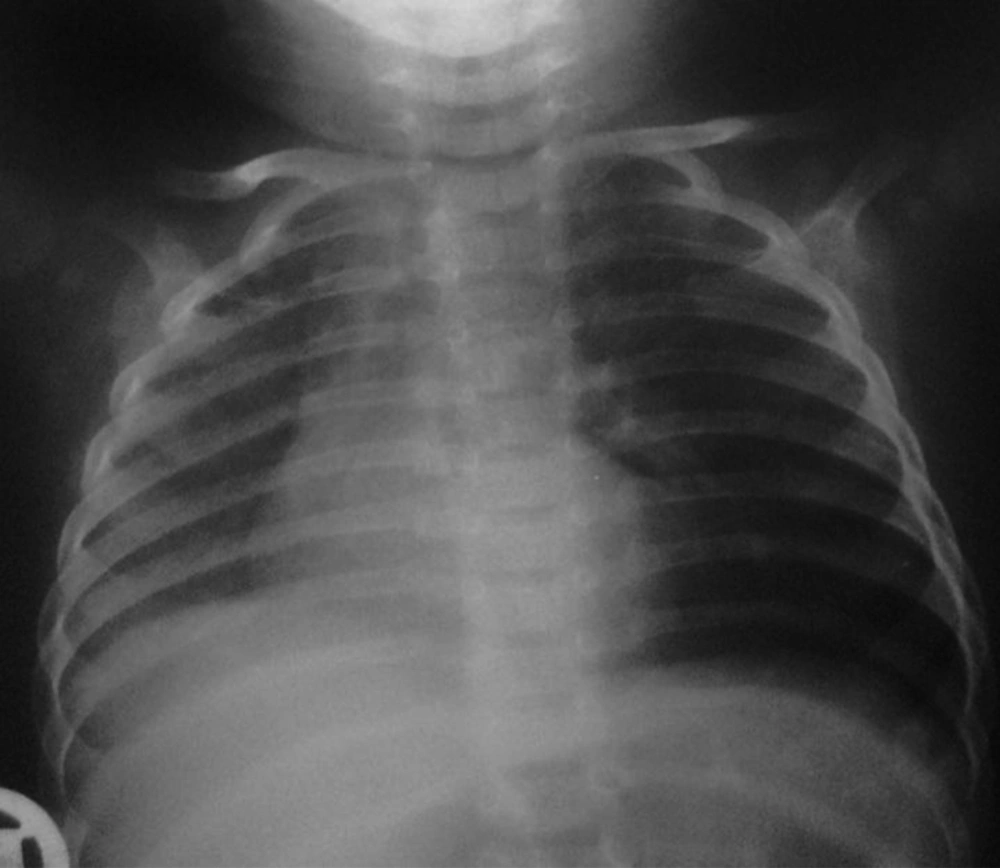
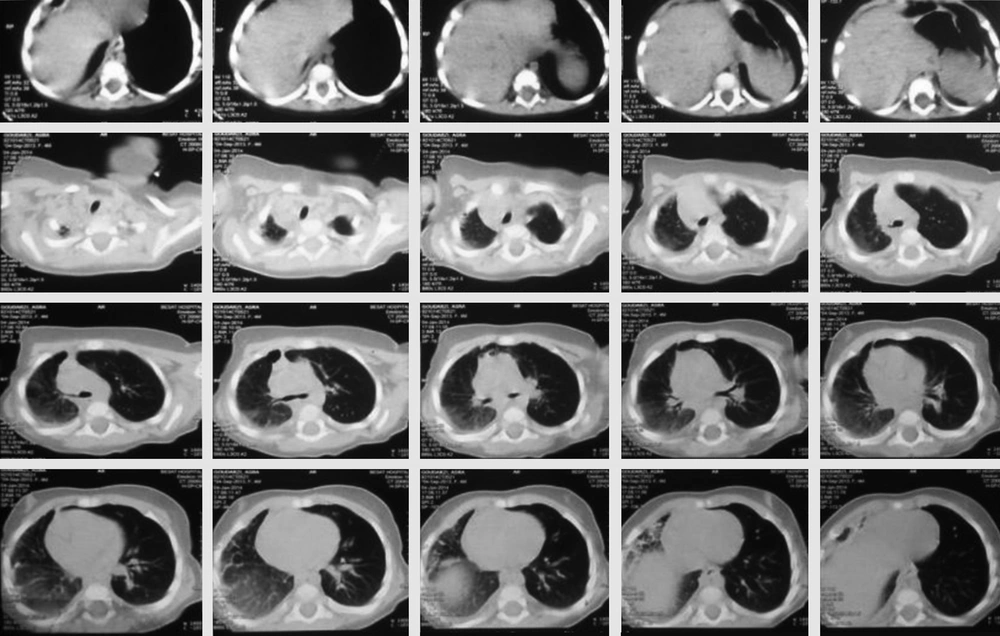
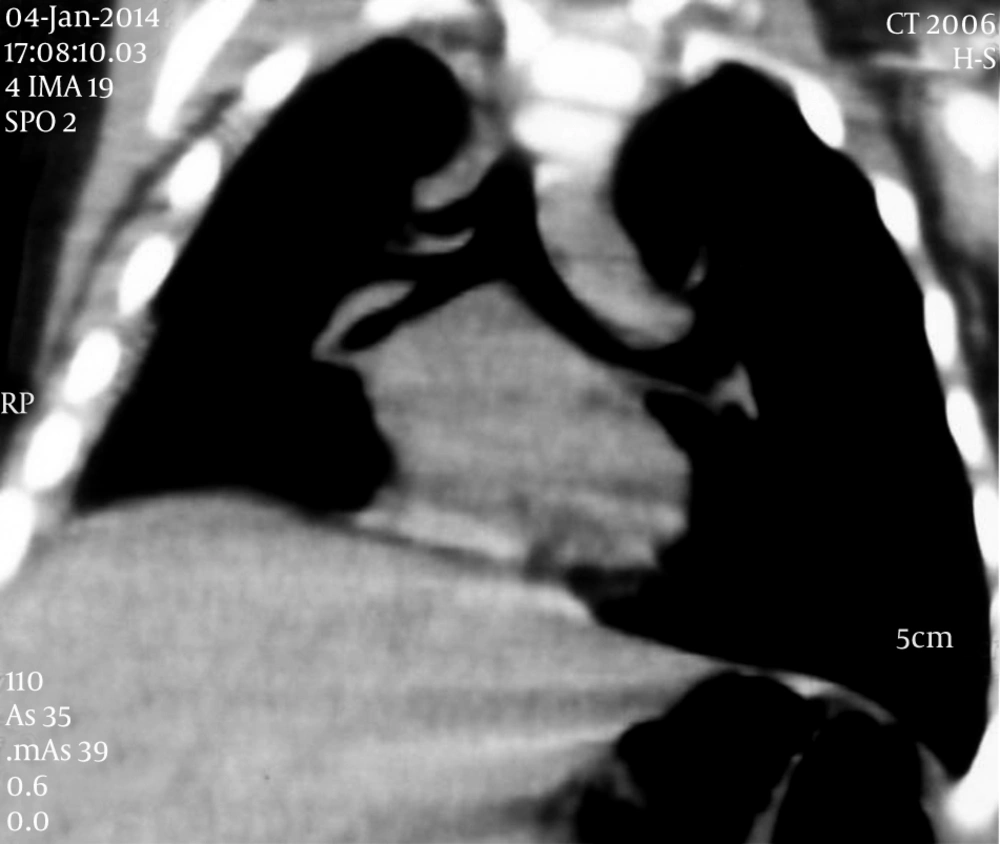
On chest X-ray, she had left lung hyperinflation and reduced volume of the right lung along with mediastinal shift to the right side (Figure 1). She underwent thorax computed tomography scan (CT scan) which revealed emphysematous changes in the apex and ground glass opacities in the middle and lower zones of her right lung and pneumonitis was suggested (Figure 2). She underwent antibiotic therapy, but because of inappropriate response to antibacterial treatment, previous history of recurrent pneumonia and further evaluation, she was candidate for bronchoscopy. On bronchoscopy, t transthoracic transthoracic transthoracic here is no foreign body, but purulent exudates and fibrin was seen in her right lung and possibility of tracheal bronchus was not proposed. Therefore, coronal view of her first CT scan was reconstructed and the presence of tracheal bronchus above the carina on right side was confirmed (Figure 3). The images of axial cuts of CT scan were reviewed one more time; it was interesting that it had some evidence for tracheal bronchus, which was missed initially (Figure 2).
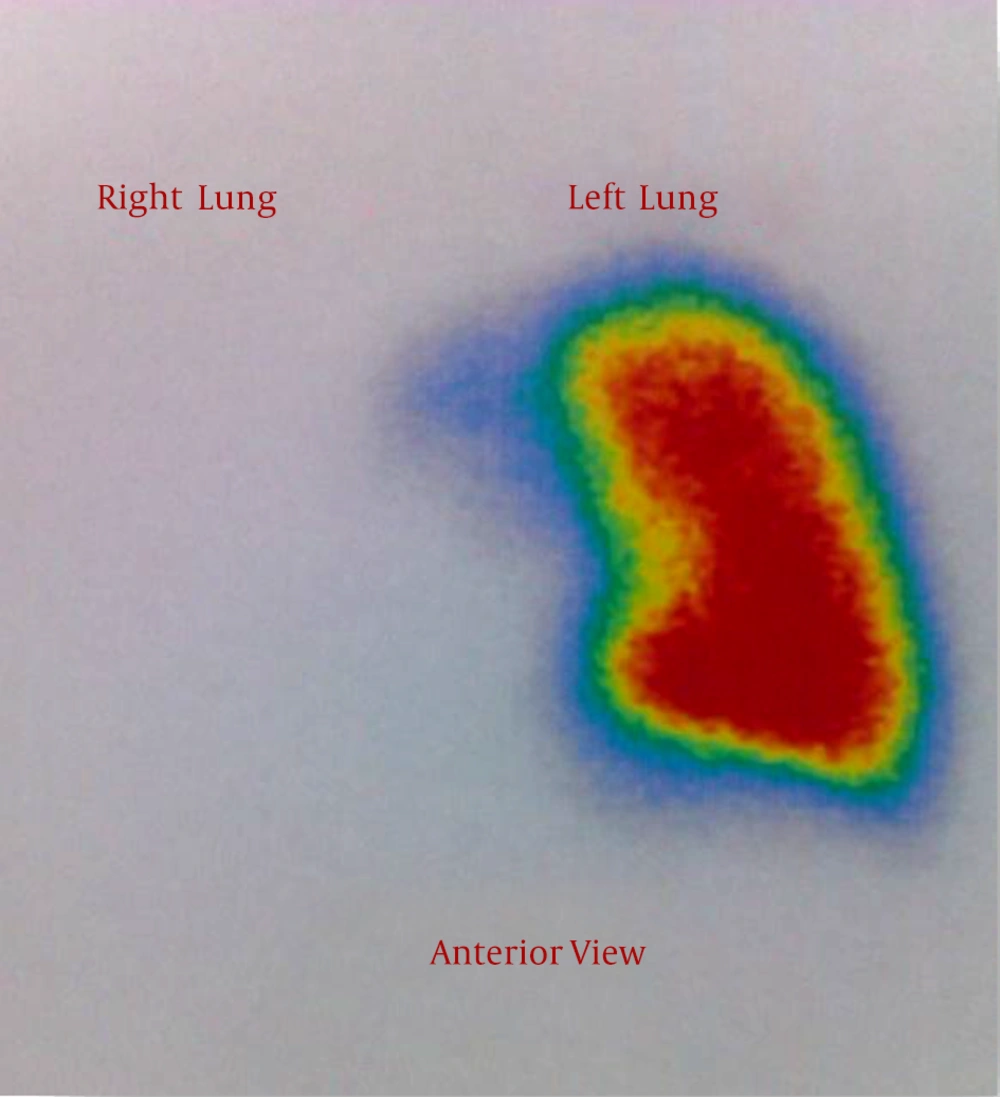
Since this pulmonary abnormality is associated with congenital heart disease, she underwent transthoracic echocardiography (TTE). Surprisingly she had no right pulmonary artery along with mild right ventricular hypertrophy. Coronary angiography was performed according to the cardiologist’s suggestion and confirmed unilateral (right) absence of pulmonary artery (UAPA). Also, lung perfusion scintigraphy was done; as expected lung scan revealed unilateral absence of right-lung perfusion (Figure 4).
The patient was referred to pediatrics lung specialist and thorax surgeon for subsequent interventions.
3. Discussion
Tracheal bronchus, first described in 1758, is a rare congenital tracheobronchial abnormality in which an ectolupic bronchus arises from the lateral wall of the trachea proximal to the carina. It originates more commonly form right side of trachea rather than left side (1). The incidence of tracheal bronchus is reported 0.1% to 3% (8).
The tracheal bronchus is classified into displaced and supernumerary types (9). In supernumerary type, the right upper lobe bronchus trifurcates and supplies the upper lobe normally and the accessory bronchus supplies an extra segment of the right upper lobe. If the right upper lobe bronchus bifurcates into two, the accessory bronchus usually supplies the apical segment of the right upper lobe and it is a displaced bronchus, which is more common than former one (1).
This anomaly is usually asymptomatic and is found incidentally during bronchoscopy or imaging done for other indications (1, 10). Sometimes it results in stridor, respiratory distress, recurrent infection, and atelectasis. Hansen-welches et al. in 2011 reported the death and babies months old infant form recurrent pneumonia due to an unidentified tracheal bronchus (11). In some patients, it is occasionally associated with difficulty in intubation due to obstruction of the bronchus orifice which results in lobar collapse (12).
In some cases, tracheal bronchus is associated with other congenital anomalies including Down syndrome, congenital heart diseases and costovertebral (5-7). Vedajallam et al. in 2013 described the five-months-old female presented with bronchiolitis finally diagnosed with tracheal bronchus and some pulmonary, hepatic and renal vascular abnormalities; among them was pulmonary sling with an anomalous left pulmonary artery originating from the right one (13). The current case was carefully evaluated for associated anomalies, which led to diagnosis of absence of right pulmonary artery. Unilateral absence of pulmonary artery (UAPA) most commonly occurs in conjunction with cardiovascular abnormalities such as tetralogy of Fallot or cardiac septal defects; however isolated cases of UAPA were reported (14).
Asymptomatic cases of tracheal bronchus do not require treatment, but surgical resection is indicated for cases of recurrent pneumonia complicated by bronchiectasis (5).
The current study patient came with episodes of recurrent pneumonia, and was diagnosed with tracheal bronchus after bronchoscopy and CT scanning. As mentioned previously, some evidence for tracheal bronchus existed in the initial axial cuts of the patient’s CT scan, but it was observed only when the cuts were reviewed as a retrograde step. Therefore the physicians are recommended to carefully explore the imaging, even for rare findings. In addition this case and other similar scenarios should sensitize pediatricians about the possibility of congenital anomalies particularly tracheal bronchus in children coming with recurrent pneumonia especially in right upper lobe; and when the diagnosis is made, associated conditions should be evaluated.