1. Background
Traditional medicine (TM) is a medical system with a long history and the knowledge, skills, and practices based on the theories, beliefs, and experiences indigenous to different cultures, which whether explicable or not, have been used in the maintenance of health, as well as for the prevention, diagnosis, alleviation, and treatment of physical and mental illnesses (1).
In this study, the term TM refers to all types of TM, including traditional Persian medicine (TPM), which involves pharmacological interventions, including the use of herbal medicines, animal parts, and/or minerals, as well as non-pharmacological interventions like manual therapies and venesection. The term complementary and alternative medicine (CAM) refers to complementary and alternative methods such as homeopathy and acupuncture that do not originate from Iran (2).
Modern medicine (MM) refers to standard medicine, which is used in healthcare systems all over the world. It includes prevention, diagnosis, treatment, and many other aspects of health. Allopathy and conventional medicine are used synonymously with MM. Integrative medicine (IM) is a comprehensive, safe, and effective approach to healthcare that combines MM with CAM and TM and is used to treat the patient’s body, mind, and even spirit. To determine the degree of the incorporation of TM/CAM into national healthcare systems, the World Health Organization (WHO) has defined some categories. The IM system represents the highest incorporation of TM/CAM into all areas of healthcare provision (1).
There are at least two main differences between MM and TPM. First, healthcare professionals in MM systems treat the symptoms of a disease while the focus of TPM is holistic and individualistic. When prescribing traditional medicine, it takes into account not only the patient’s all ailments but also their characteristics like lifestyles and living environments. Traditional Persian Medicine is, in fact, similar to precision medicine, which is being promulgated these days (2). Second, while in MM, every medication has one active substance with a special pharmacological characteristic, herbal medicines contain several substances, the combination of which is responsible for their efficacy.
Given the origin of TPM that goes as far back as 7000 years, and the fact that it was the main medical paradigm in a vast geographical area of the world as far afield as India, Europe, and North Africa until as late as the Renaissance, it is; therefore, little wonder why TPM is held in a high regard by many Iranians (2, 3). In Iran, Amir Kabir, the first prime minister of Naser al-Din Shah Qajar, introduced some major reforms in medicine, including the foundation of Dar ul-Funun school in 1851. Obliging practitioners to obtain a license for their practice was another of his legacies (4). Before these reforms, treatments were limited to TPM.
Although the medical system has been based on modern medicine recently, Iranians’ inclination toward TPM remains intact. Of course, TPM is used along with modern medicine (MM) for treating patients in Iran’s healthcare system. A study in Kerman, the largest city in the southeast of Iran, revealed that 88.4% of diabetic patients had used at least one CAM/TM treatment in the past year. The most common treatment was the use of herbal medicines, which had been tried by 84.9% of the patients (5). Another study in Shiraz showed that 97.7% of diabetic patients had used herbal medicines (6). In a study evaluating the use of CAM/TM for epileptic children in Tehran, it was found that 44% of parents had used CAM/TM methods either alone or in combination with other methods, and only 16.7% of these parents had told their children’s physicians about their use of CAM/TM (7). Increasing demand for TPM led to the establishment of Ph.D. courses for physicians and pharmacists in this field in Iran in 2007, followed by the establishment of TPM clinics for providing healthcare services to patients.
Nowadays, medicinal plants are used in three ways to treat diseases in Iran. First, they are used in MM dosage forms such as tablets, syrups, ointments, and drops, which are distributed in pharmacies. They are either prescribed by a physician or are available over the counter (OTC). Second, TPM drugs are produced based on the regulations of the preparation and distribution of TPM products approved in December 2006. They are usually prescribed by TPM specialists. Finally, medicinal plants are used as self-medication in bulk and provided by traditional herbal shops called “Attari”. These shops do not operate under the control of the health ministry. To run an Attari, one does not need to apply for a particular license or is not required to hold an academic degree.
Regardless of the type of the medication taken, for it to be effective, it must be taken correctly, which means that the patient must follow standard therapies instructions, highlighting the importance of "medication adherence". Medication adherence may influence treatment outcomes, which explains why this is an important variable in any therapeutic attempt. Non-adherence to medication negates the effects of the treatment process, which may inevitably deteriorate the patient’s condition and incur unnecessary medical costs and even death (8). Even participants in approximately 30% of clinical trials with a controlled and accurate condition miss doses. It can worsen the conclusions of clinical trials (9). The positive correlation between low adherence to medication and poor quality of life further justifies the importance of medication adherence in treatment protocols (10).
A 2003 WHO report defined adherence as "the extent to which the patient follows medical instructions" (11). The concept of adherence deals with the patient’s voluntary involvement in the treatment process, where they play an active role in achieving therapeutic goals by following an agreed course of treatment and sharing responsibility with healthcare providers (11). However, there is widespread confusion surrounding adherence to medication and compliance with medication, and these concepts are sometimes used interchangeably. This confusion has to be cleared in order to put things into perspective. While adherence refers to the patient’s commitment to the physician’s recommendations, compliance implies the patient’s passivity in the treatment process (12). In other words, compliance means that patients follow what the doctor has decided while the patient has medication adherence when they choose the type of treatment and adhere to their desired prescribed therapeutics. Unintended non-adherence can occur when patients think they are adhering to the treatment, but actually they are non-adherent because of a deficiency in knowledge or skill (11).
Although adherence to TM may not be taken seriously, it is a really important issue. On the one hand, some traditional medications are not available in modern dosage forms, which can confuse the patient. In fact, because of the appearance of the medication, the patient might labor under the misapprehension that this medication does not have to be taken as regularly as modern medications. On the other hand, it is used along with modern medications, and an element of caution should always be exercised as to the indications, adverse effects, drug interactions, and contraindications associated with the concurrent use of TPM and MM.
Some people’s high tendency to TPM begs the question of what factors can affect their tendency, and how this tendency can contribute to their adherence. The rates of adherence may vary depending on disease nature, demographic features of patients, and the types of medications. However, non-adherence is a general problem, and the importance of figuring out an optimal solution to both TPM and MM cannot be more strongly emphasized (13). Against this backdrop, this study was designed to evaluate the factors affecting adherence and non-adherence to TPM. In order to plan for integrative medicine as a program addressing different health needs and promoting public health and patients’ quality of life, all the factors affecting people’s tendency to use TPM and their adherence should be taken into account, and if necessary, some timely interventions should be considered.
Policymakers should understand how TPM can improve people’s health in the modern healthcare system. Patients, physicians, pharmacists, policymakers, etc., are different stakeholders whose opinions should be considered in decision-making.
2. Objectives
We aimed to investigate patients’ perspectives and evaluate the factors affecting their tendency and adherence to TPM. Among different practices of TPM, we focused on herbal medicines.
3. Methods
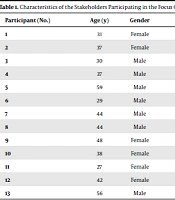
In this qualitative directed thematic analysis study, a purposeful sampling technique was employed to look for information-rich cases. One focus group with in-depth interviews with 13 people and four in-depth interviews were conducted (Tables 1 and 2). Although 6-12 people are required as the standard size of a focus group discussion (FGD), it is advisable to over recruit by 20 - 50% as some people may face a problem or change their minds about participating in FGD. In this study, all 13 invited people attended the meeting (14, 15). A FGD method was used to discuss the feelings, perceptions, and beliefs of different stakeholders about TPM in detail; this was done because little is known about stakeholders’ perspectives on TPM in Iran (16). Individual in-depth interviews were also conducted to validate and enhance the accuracy of the interviews and to reach the saturation point. The saturation point was reached in the fourth interview, and no new information was obtained after the last one.
| Participant (No.) | Age (y) | Gender | Education | Status |
|---|---|---|---|---|
| 1 | 31 | Female | Pharm. D | Community pharmacist |
| 2 | 37 | Female | Ph.D. | Clinical pharmacist |
| 3 | 30 | Male | Ph.D. | Pharmacognosist in industry |
| 4 | 37 | Male | Ph.D. | Pharmacoeconomist (Researcher) |
| 5 | 59 | Male | MD | General practitioner |
| 6 | 29 | Male | Ph.D. | Neurologist |
| 7 | 44 | Male | Ph.D. | Pharmacognosist (Policy-maker) |
| 8 | 44 | Male | Ph.D. | Pharmacoeconomist (Policy-maker) |
| 9 | 48 | Female | Pharm.D | Policy-maker |
| 10 | 38 | Female | Ph.D. | Traditional pharmacy specialist (Academic) |
| 11 | 27 | Female | B.S. | Patient |
| 12 | 42 | Female | High school diploma | Patient |
| 13 | 56 | Male | High school diploma | Attar |
| Participant (No.) | Age (y) | Gender | Education | Status |
|---|---|---|---|---|
| 1 | 37 | Male | Ph.D. | Traditional medicine specialist (Policy maker) |
| 2 | 29 | Male | Ph.D. | Pharmacognosist researcher |
| 3 | 41 | Male | Ph.D. | Traditional pharmacy specialist (Academic) |
| 4 | 47 | Male | Ph.D. | Traditional medicine specialist |
The individuals participating in a FGD may be homogeneous for some features and heterogeneous for others (14). In this research, we included TPM stakeholders, so they were homogeneous in being a TPM stakeholder and heterogeneous for a number of other characteristics, situations, and experiences with the phenomenon under study.
The participants included a general practitioner, a pharmacist, a neurologist, a clinical pharmacist, a traditional pharmacist, a traditional medicine specialist, two patients taking traditional medication, three policymakers, an academic in the field of traditional and natural medicines, a person working in the natural medicine and TPM industry, an Attar (a person running an Attari), two pharmaco-economists, and a pharmacognosy specialist. (Tables 1 and 2).
The principal investigator, who received training about the qualitative methodology and interview process, directed focus group discussions and interviews. The interviews were conducted in Farsi (Iran’s official language). The focus group interview lasted about three hours, with a 15-minute break midway through. A variety of snacks and drinks were served at the time so that people could continue discussions better. Although the participants were suggested to take part in two sessions, they preferred one. Time, cost, and the availability of participants are the factors limiting the number of sessions that can be held (14). The individual interviews also lasted 25 - 45 minutes each. All the interviews were recorded, and the respective audio files were subsequently transcribed verbatim. The principal investigator analyzed the data using MAXQDA 2018, a qualitative data analysis software, read the texts to understand the data, and then broke down the data into smaller units (codes). Next, the codes were clustered to create sub-themes that were in turn clustered back into main themes (17). For verifying the validity of the study, the main themes and codes were sent to the study participants to approve them. Some direct quotations from the participants have been provided on the following pages.
Because the data collected were only based on the participants’ ideas and experiences, and the fact that no medical records were collected, the study did not need an ethical committee’s approval.
4. Results
The results of this study revealed a variety of factors affecting people’s adherence to TPM. During the focus group and interviews, the participants discussed how these factors affected their adherence to traditional and natural medicine. Patients’ desire to use TPM was noted to have an impact on their adherence to TPM, indicating that the factors affecting adherence are the same factors affecting compliance, which can be combined with the factors affecting patients’ tendency to take these medications.
Once the interviews were analyzed, four main themes affecting tendency and compliance were extracted. These main themes included popular beliefs, the inherent characteristics of TPM and its status quo, attempts to bring about positive changes to TPM, and problems facing the modern health system (Tables 3 and 4). More specifically, 134 codes and 15 sub-themes were obtained regarding the factors affecting compliance, which were then classified into four themes with positive effects and three themes with negative effects on compliance. On the other hand, 163 codes and 14 subthemes were extracted as the factors affecting the tendency, which were then classified into four themes with positive effects and three themes with negative effects on tendency. Some degrees of overlap were observed between the negative and positive categories.
| Themes | Subthemes | Number of Codes Related to Each Theme | |
|---|---|---|---|
| Positive Effects on Compliance | Negative Effects on Compliance | ||
| Popular beliefs | Belief in the cost-effectiveness of TPM | Unreliable effectiveness | 42 |
| Belief in the safety of TPM | Unreliable safety | ||
| Patients’ desire to overuse medicines | Not considering herbal medicine as real medicine | ||
| Inherent characteristics of TPM and the status quo | Increased satisfaction | Financial burden | 71 |
| Difficulties of TPM treatment | |||
| Some TPM practitioners damage people’s trust in TPM | |||
| Attempts to bring about positive changes to TPM | Better patient education | 13 | |
| Promotion of formulations similar to modern medicine | |||
| Problems facing the modern health system | The last treatment option | Fear of disagreement with modern medicine practitioners | 8 |
| Side effects of chemical medicines | |||
| Themes | Subthemes | Number of Codes Related to Each Theme | |
|---|---|---|---|
| Positive Effects on Tendency | Negative Effect on Tendency | ||
| Popular beliefs | Psychological effects | Individual differences | 40 |
| Individual differences | |||
| Inherent characteristics of TPM and the status quo | Holistic | Lack of an appropriate inspection of Attaris | 35 |
| Simultaneous use of traditional and modern medicine | Unprofessional opinions in the field of TPM | ||
| The complexity of the problem of TPM clinics’ patients | |||
| Attempts to bring about positive changes to TPM | The patient’s good feeling | - | 75 |
| Suitable behavior of TPM practitioner | |||
| Appropriate time for physician-patient communication | |||
| Problems facing the modern health system | Stubborn adherence to the status quo | Fear of disagreement with modern medicine practitioners | 13 |
| Mistrust of the modern health system | |||
4.1. Popular Beliefs
Popular beliefs play both positive and negative roles in adherence. These notions may affect people’s actions, their personality, habits, emotions, individual differences, feelings. The psychological effects of the patient-physician communication are interpreted as beliefs. Popular beliefs are at the heart of their personality. Popular beliefs can change, so can their personality (18). In what follows, a number of TPM stakeholders have been directly quoted to put their beliefs more into perspective.
4.1.1. Positive Effects on Compliance
4.1.1.1. Belief in the Cost-effectiveness of TPM
A TPM expert said: TPM has a holistic view of diseases. An example is dandruff. If a patient with dandruff, suffering from some diseases, wants to cure all his/her problems with MM, he/she needs to see a specialist for each disease and pay more money for visiting and purchasing medicines. However, if these patients visit a TPM specialist, they get a more lasting result by the long-term and correct use of TPM. You should not be worried about short-term costs. Rather, think of the long-term costs and the effects.
4.1.1.2. Belief in the Safety of TPM
A patient said: Even assuming that TPM does not work, at least, it is not harmful.
4.1.1.3. Patients’ Desire to Overuse Medications
A TPM practitioner said: We do not care about interactions. Physicians over-prescribe medicines, which means there must be something wrong with MM. Once I had a patient who was taking 45 medications a day. Patients are getting used to being over-prescribed. They prefer a system that encourages them to take more medicine.
4.1.2. Negative Effects on Compliance
4.1.2.1. Unreliable Effectiveness
4.1.2.1.1. Non-standard
A pharmacognosist said: The essence of herbs is variable; they constantly change as nature does. The plant that grows is variable, which results in a variety of active ingredients.
4.1.2.1.2. Belief in the Inefficacy of Nutraceuticals
A policymaker said: TM is in a subordinate position. Therefore, the patient’s expectation of its efficacy is low. A familiar refrain is “I either get better or get nothing”.
4.1.2.2. Unreliable Safety
A policymaker said: Sometimes, different manufacturers offer different compounds with the same name. Because it is not standard; it is not necessarily industrial; therefore, taking the right medicine is riskier.
4.1.2.3. Not Considering Herbal Medicines as Real Medicines
A patient said: We do not often feel that it is a medicine. It may be easier to change the time of the administration of a medicine unconsciously. However, we get used to using chemical medicines on time, especially antibiotics.
4.1.3. Positive Effects on Tendency
4.1.3.1. Psychological Effects
A participant said: In my opinion, the bitter taste is a positive thing in TPM. In the past, sometimes herbs did not work, but they were bitter. The patient thought this bitter medicine would heal their diseases.
4.1.3.2. Individual Differences
A patient said: Most women are more persistent and determined than men and resign themselves to the hardships involved in herbal medicine consumption; for example, they are more willing to go through the rigmarole of preparing the concoction and face the unpleasant prospect of drinking it several times a day at unforgiving intervals.
4.1.4. Negative Effects on Tendency
4.1.4.1. Individual Differences
- A patient said: My cousin told me, “I cannot eat these things that you eat. Look at its color! Look at the appearance!”. Such attitudes can be inherently repulsive and deter patients from using this medicine.
- A traditional pharmacist said: Although some patients prefer the whole plant, others prefer formulations like a capsule.
4.2. Inherent Characteristics of TPM and Its Status Quo
The inherent characteristics of TPM and what is known as the TPM system these days may have an impact on patients’ adherence. The holistic approach of TPM, its natural aspect, and how it has been passed down from generation to generation constitute the inherent characteristics of TPM. Financial issues, difficulties in consuming herbal medicines, and related policies collectively constitute the notions of the status quo.
4.2.1. Positive Effects on Compliance
4.2.1.1. Increased Satisfaction
A TPM practitioner said: Cancer is the best example for using IM. We are practicing both TPM and MM in a cancer institute. The concurrent use of TPM and MM improves patients’ quality of lives.
4.2.2. Negative Effects on Compliance
4.2.2.1. Financial Burden
A pharmacoeconomist said: Because these medicines originate from plants, any price, however much, is high from the patient’s point of view. In their opinion, despite that these medicines are domestic, their prices are nearly as much as those of imported ones.
4.2.2.2. Difficulties in TPM Treatments
Misuse, difficulties in access, having no special formulation, long-term and frequent use, needing to be prepared by the patient, incompatibility with today’s lifestyle, and the usage of various medications are some important difficulties associated with TPM treatments.
Some stakeholders’ opinions on difficulties in ITM treatments are as follows:
- One patient said: The volume of herbal distillate is high. For example, on a trip, you have to carry four containers of herbal distillate, and you may spill it and ruin your suitcase.
- Another patient said: Sometimes you have to stay home to prepare the medicine. A drug should be taken an hour before a meal, in the middle of the meal, and you should brew this once again. This is impossible in modern life.
- A policymaker said: Some TPM practitioners damage people’s trust in TPM. Conflict of interest is a pressing issue. A physician should not have any vested interest in the sales of medicines because it can affect their diagnosis.
4.2.3. Positive Effects on Tendency
4.2.3.1. Holism
A TPM expert said: We prescribe one medication, which cures all ailments.
4.2.3.2. Concurrent Use of Traditional and Modern Medicine
A TPM pharmacist said: When MM is used to treat fatty liver, and it fails, the patient turns to TPM. After two months, they take a laboratory test for their liver enzymes. In TPM, we also use new diagnostic tools. TPM specialists do not rely only on what is in their references and ancient books.
4.2.3.3. Complex Problems of TPM Clinics’ Patients
A TPM practitioner said: A person who comes to a TPM clinic has visited other doctors and has been given medications that have not helped them much. Nobody visits a TPM expert just to correct and improve his/her lifestyle.
4.2.4. Negative Effects on Tendency
4.2.4.1. Lack of Appropriate Inspection of Attaris
A person working in natural medicine and the TPM industry said: If Attaries become organized by the health ministry, people’s trust in them will grow, and they will return to them for medications more and more.
4.2.4.2. Unprofessional Opinions in the Field of TPM
A neurologist said: There is widespread confusion when it comes to differentiating evidence-based TPM from the one lacking any evidence. This melting pot of pseudoscience and evidenced-based TPM can harm TPM’s reputation.
4.3. Attempts to Bring About Positive Changes to TPM
Any effort to improve the situation of TPM has positive effects on people’s compliance and desire to use this type of medicine. The participants talked about the positive effects of educational courses in medical schools for physicians, educating patients, and the patient-physician relationship, which could affect patients’ satisfaction and promote their adherence to TPM (19).
4.3.1. Positive Effects on Compliance
4.3.1.1. Better patient education
A TPM pharmacist said: The Persian word "Bokhur", pronounced as “Bookhoor”, which means using vapors of some herbal brew, is a homograph of another Persian word, "Bokhor", pronounced as “Bokhor”, meaning "eat". This seemingly innocuous formal similarity has had some disastrous consequences when patients have orally taken a medicine that was supposed to be inhaled or smelled instead. Traditional pharmacists advise patients on the preparation of their medicines to iron out any potential misunderstandings in advance.
4.3.1.2. Promotion of Formulations Similar to MM
One patient said: My physician prescribed capsules for my knee pain, which I found easier to use than brewing.
4.3.2. Positive Effects on Tendency
4.3.2.1. Patients’ Good Feelings
These good feelings include a sense of intimacy, comfort, security, and trust when a medicine is prescribed by a physician and supplied by the healthcare system.
- A patient said: TPM doctors’ behavior is very friendly to me. They are like psychologists because they get a patient’s history, habits, the foods and medicines they eat, which may take up to 45 minutes.
- A person working in the natural medicine and TPM industry said: Our people are looking for stylish and packaged medicines nowadays.
4.3.2.2. TPM Practitioners’ Appropriate Behavior
- A patient said: It is more important to accompany the patient than treat them.
4.3.2.3. Allocating Adequate Time for Physician-patient Communication
A pharmacist said: When a patient speaks to a doctor for 45 minutes, the doctor sounds more credible to them than the one who prescribes medications without asking for the patient’s history.
4.4. Problems of the Modern Health System
The participants mentioned some problems for modern medicine encountered by patients in the healthcare system. When patients experience side effects with chemical medicines or do not have an alternative therapeutic option, they may turn to TPM. Sometimes doctors do not agree with this choice, which can meddle with patients’ adherence.
4.4.1. Positive Effects on Compliance
4.4.1.1. The Last Treatment Option
A pharmaco-economist said: Patients who choose TPM are those who are disappointed with modern treatments.
4.4.1.2. Side Effects of Chemical Medicines
One patient said: I was taking corticosteroids for my knee pain. This tripled my weight, and, as a result, I developed atherosclerosis. I could not move my legs without taking corticosteroids, but with TPM, I gradually reduced my corticosteroids, and I have not used corticosteroids for over a year now and also have no movement problems.
4.4.2. Negative Effects on Compliance
4.4.2.1. Fear of Disagreement with MM Practitioners
A TPM physician said: A patient took a lot of medicines separately prescribed by a rheumatologist, neurologist, cardiologist, and an internal specialist. I sent him to two clinical pharmacists, and no one dared to modify his medications.
4.4.3. Positive Effects on Tendency
4.4.3.1. Stubborn Insistence on the Status Quo
A patient said: When some physicians insist that I should not use MM, they indeed stand to benefit from it personally. Maybe they are importing some medicines that they would like their patients to use.
4.4.3.2. Mistrust in the Modern Health System
A patient said: In MM, they scratch each other’s back. When a doctor says you need sonography or a laboratory test and insists on a special sonography center or lab, the patient starts smelling a rat. This can cultivate a miasma of distrust, profiteering, and dishonesty.
4.4.4. Negative Effects on Tendency
4.4.4.1. Fear of Disagreement with MM Practitioners
Patients worry that their doctors may refuse to treat them when they learn about their use of TPM.
5. Discussion
This study aimed to explore the factors affecting patients’ adherence to TPM and found that adherence to TPM is multifactorial, and people’s beliefs, the inherent characteristics of TPM and its status quo, attempts to bring about positive changes to TPM, and the problems facing the modern health system play a crucial role in this regard.
According to the results, the factors affecting patients’ adherence can be broadly categorized into two groups: patient-related and environment-related factors. Regarding patient-related factors, socioeconomic parameters and the items arising from individual differences and manners can affect adherence. In this case, policymakers may not be able to interfere directly, or the change may take a long time, but any intervention in environmental factors by policymakers (i.e., status quo, attempts to bring about positive changes to TPM, and the problems facing MM) can directly affect medication adherence.
In other studies, adherence or non-adherence to medications has been described as a multifactorial issue, suggesting the complexity of the nature of adherence. In a study, Jimmy et al. stated that non-adherence is a common phenomenon in all the patients receiving medicines, and the complexity of this phenomenon is due to the interaction of various factors such as patients’ approaches and behavior, disease characteristics, social factors, accessibility, and the quality of services (8). In another study, Parra et al. evaluated the factors contributing to adherence to therapeutic regimens in hypertension and diabetes and found that health-system related factors could discourage adherence, while some therapy-related factors can promote it (20).
By definition, an adherent patient has an active role in achieving therapeutic goals, so it seems that a patient’s tendency is crucial in adherence. In other words, if patients’ tendency and compliance converge, adherence would be achieved. Therefore, all the factors affecting patients’ desire and compliance were extracted from in-depth interviews to show the forces driving patients’ adherence.
In this study, we considered TPM because of its critical role in IM. Health-related quality of life and satisfaction could be improved through IM in the healthcare system (21, 22). The importance of TPM in the comprehensive scientific map of Iran has led to the development of a national document on medicinal plants and ITM of the Islamic Republic of Iran (23, 24). A part of the prospects of this document states that Iranian traditional and herbal medicine should flourish, innovate, and play an effective and prominent role in the country’s health system through the use of evidence-based, safe, high-quality, effective, and accessible services to the community (24). Although policymaking on the integration of TPM in Iran has been considered, the adopted policies either are being implemented too slowly or have fallen into abeyance (25).
Herbal medicines often need preparation and usually need to be used for a long period. Sometimes they are used as a flavor, a hot drink, or food in our everyday life. These characteristics may encourage non-adherence vis-à-vis MM. Therefore, divulging the factors that influence patients’ adherence to these medicines can show the extent to which current policies are in line with patients’ desires and the changes that should be made to improve the status quo.
What is considered “people’s beliefs” in this study is partly related to people’s personality, habits, individual differences, feelings, and the psychological effects of patient-physician communication that can change if enough time and attention are allowed. Patient satisfaction and positive patient experience are a function of a healthy patient-physician relationship (26, 27). In a study by Kristoffersen et al., socio-demographic characteristics that make individual differences, such as education, age, socioeconomic status, and religiosity, were associated with the use of TM (28). Other studies show that education and governmental leadership can positively change popular beliefs (29).
Regarding the role of popular beliefs in the efficacy and safety of TPM, clinical trials and animal studies can moderate over-trust and mistrust, leading to adherence and non-adherence, respectively. In that case, popular attitudes toward the safety and efficacy of a medication would be based more on logic than on emotions. Marketing techniques can also change popular beliefs (30). Although plans for changing popular beliefs should be in order, it seems that focusing on other factors that can improve patients’ adherence should take precedence. As beliefs might change over time based on the experiences one gains, this change may sound somehow unlikely (18).
In terms of the inherent characteristics of TPM, the TPM’s holistic approach, for example, means that it can cure several diseases in one person by modifying his/her temperament. In addition to the feelings that nature and plants create in the patient, this feature can increase patients’ tendency to take these medications.
Given its over-reliance on words of mouth and anecdotal evidence, TPM harbors the risk of throwing pseudoscience into a field mainly characterized by a strong scientific track record. Therefore, some people’s mistrust of this medicine should by no means come as a surprise. Besides, problems with using unformulated forms, such as the difficulty of consuming the right amount of the medication, can encourage non-adherence (31).
The current situation is also due to historical trends and policymaking so far. In service delivery, there are problems with supply, especially in bulk orders and when Attaries are responsible for delivery. Conflict of interest of some TPM practitioners can also cultivate a sense of distrust and cynicism. Financial problems such as high prices and lack of insurance may further aggravate the situation (32). All these factors can eventually foster non-adherence. The current situation needs to be modified by focusing on the TPM field.
For example, an attempt happened at the end of 2019 to modify the situation. The Supreme Council of Health Insurance of Iran decided to cover TPM practitioners’ fees for one year as a pilot program. However, as drugs were expensive, they were excluded from this program. Policymaking with evidence-based tools such as cost-effectiveness analysis, education, and providing a suitable situation for IM may improve the status quo.
Some of the factors causing non-adherence have improved in recent years. The introduction of medications in the form of tablets, capsules, and other dosage forms, which are easier to be used than concoctions, and the fact that patients are not required to prepare anything special should be hailed as positive steps toward encouraging adherence.
In MM, there are many reasons for non-adherence, some of which are associated with drug formulations, complex regimens prescribed by multiple physicians, long disease duration, and comorbidities (33). Approaches such as fixed-dose combinations formulated as "polypill" and extended-release formulations have been proved to be efficient in increasing medication adherence (34, 35).
The WHO in TM Strategy 2014-23 recommends evidence-based healthcare education on traditional and complementary medicine (T&CM) for healthcare providers (1). Related education curricula and T&CM educational courses in medical schools have been improved in the last decade all over the world, but there are variations in teaching methods (2, 36-42). Instructors and healthcare providers can help them recognize and differentiate science from pseudoscience to make the best of TPM. One of the most important barriers to T&CM education is the lack of evidence to support CAM applications (36).
Other positive effects of recent efforts are patient education and the patient-TPM physician relationship guaranteeing patient satisfaction. In TPM clinics, a healthy relationship has been observed between patients and healthcare providers. This improvement in communication results from TPM clinic rules and the consideration of the physician-patient relationship in professional TPM educational courses.
Physician-patient communication has been studied extensively because of its importance in patients’ health outcomes (19, 43). Pharmacist-patient interaction also increases patients’ knowledge and satisfaction (44). Paying attention to a patient’s emotions can play a critical role in patient satisfaction and, consequently, better outcomes (31). The last extracted theme in the present study included the problems of the modern health system. Some people are looking for a place to escape from the modern health system (32). If TPM is not a good safe haven for patients, what will happen to them?
Sometimes the patients referred to TPM clinics have not responded to MM or have turned to TPM because of the side effects of chemical drugs. In many cases, TPM can do nothing in the treatment of these patients. Patients should be aware that TPM can sometimes help treat them, but sometimes it only improves their QOL.
Some patients doggedly fight the status quo or do not trust the existing healthcare system. Evidence-based and culturally-tailored interventions may overcome this sense of mistrust and improve adherence (45). Fear of disagreement with physicians who are against TPM and do not continue to treat patients may lead patients to give up on TPM.
There is no shortage of studies addressing TPM in Iran alongside evidence-based medicine. Moreover, medical education is being promoted in this field. However, it seems that other platforms are yet to be provided for its further development and promotion.
However, the findings of this study should be interpreted with caution as, similar to many other studies, it has a number of limitations. Perhaps, the most important limitation is the relatively low number of participants in this study, hindering its applicability and generalization to broader contexts. Conducting a similar study with a greater number of participants can go a long way toward ensuring its validity.
5.1. Conclusions
This study provides important insights into the effect of adherence to TPM on patients’ health outcomes through extracting the factors affecting adherence and non-adherence to TPM medications. If patients’ tendency and compliance converge, adherence would be achieved. Therefore, adherence necessitates the existence of several factors. Among others, popular beliefs, the inherent characteristics of TPM and its status quo, attempts to bring about positive changes to TPM, and the problems facing the modern health system are reasons that can influence adherence and non-adherence. These results can guide policymakers for further interventions in the field of integrative medicine by removing barriers and focusing on strengths. More research on TPM is necessary for the development of IM in Iran.