1. Background
Simulation-based education (SBE) is an educational technique, which aims to create an environment resembling real-world experiences (1). It encompasses a wide range of modalities, including technical training and deliberate practice using part-task training models, simulated patients, and immersive simulation scenarios with an array of low- to high-fidelity manikins and technology. In healthcare education, SBE is usually employed to enhance the training of participants or for the purposes of evaluation (2). While numerous learning theories underpin immersive SBE, Kolb’s experiential learning theory is often cited by simulation educators as the most suitable model (1-3). By using realistic simulated experiences followed by periods of active reflection on their experiences and their peers’, immersive SBE allows learners to actively construct knowledge and understanding by linking new information to previously constructed schemata (4). With appropriate faculty expertise and guidance during the debriefing process, learners can explore how any new or altered notions can be applied in similar future situations, in which a new cycle of experiential learning can take place (1, 2, 4). Also, immersive SBE helps achieve a safe learning environment where patient safety cannot be compromised (1, 2).
Medical students are scarcely exposed to acutely unwell pediatric patients (5) due to several barriers, such as limited time in undergraduate pediatric clinical blocks, reduced incidence of acutely unwell pediatric patients, and ethical considerations surrounding parental consent and patient safety (5-7). Concerns regarding patient exposure and clinical risk during the COVID-19 pandemic will only exacerbate this problem. Thus, it is necessary to find innovative methods to overcome these barriers, and immersive SBE is one such method. This method ensures that medical students gain exposure to acute life-threatening pediatric emergencies in a safe and effective learning environment.
While immersive SBE has been widely adopted in postgraduate pediatric training (1-7), its use in delivering aspects of the undergraduate pediatric curriculum in the UK is limited with little published data currently available (5-8). This is despite a growing evidence-base describing the benefits of immersive SBE, across multiple specialties in the undergraduate population (2, 6).
The present study reports the development, implementation, and evaluation of a multi-center immersive Simulation of Pediatric Life-threatening Emergency Scenarios (SimPLES) course for medical students in the west of Scotland.
2. Objectives
The current study aimed to establish a multi-center immersive simulation experience for undergraduate medical students to bridge the previously-discussed gaps. We sought to increase students’ exposure to acutely unwell pediatric patients, improve their understanding of the importance of non-technical skills (NTS) within the clinical workplace, and provide practical experience of tasks such as prescribing. Furthermore, while exploring their perceptions and opinions of the course, we sought to evaluate whether or not the course affected the students’ confidence in assessing and managing acutely unwell pediatric patients.
3. Methods
Merely six conditions account for over 80% of emergency pediatric medical presentations (9). To reflect this, we developed the following five common clinical scenarios: meningococcal septicaemia, croup, asthma, bronchiolitis, and febrile seizure. To ensure quality assurance, all scenarios were designed and written by an experienced pediatric teaching fellow together with a senior clinical simulation fellow formally trained in simulated scenario design.
Six to nine students attended each course. They were pre-briefed and orientated to the simulation environment as advocated by international consensus guidelines (10). They then received two short tutorials regarding the principles of the A-E assessment and fluid management and prescriptions in pediatric patients. Then, they participated in the immersive simulation scenarios. We used low-fidelity manikins with portable iSimulate kits, controlled by an in-situ facilitator. Two students actively participated in each 10-minute scenario, with the remainder watching in a remote location via an audio-visual link. One scenario included a simulated patient encounter with a faculty member who is playing the role of a distressed parent. Each scenario was followed by a 20-30 minute structured debriefing led by two faculty members formally trained in simulation debrief and co-debrief facilitation techniques (11). Each debrief focused on the importance of NTS in the clinical workplace. It was followed by a short five-minute mini-tutorial focusing on the technical and pathophysiological aspects of the particular clinical presentation. While adding such mini-tutorials is not common within immersive SBE, their inclusion was based upon previous experience and feedback from medical students’ regarding their individual and collective learning needs. Each course required a minimum of three trained faculty to run.
We used a mixed-method research methodology to evaluate the impact of the course. Firstly, we used a 5-point descriptor scale, ranging from ‘not at all confident’ to ‘not confident’ to ‘neutral’ to ‘confident’ to ‘very confident’. These descriptors were converted to numerical values between one and five for quantitative analysis, using a paired students t-test. The normality of data was verified with skew values consistent with a normally-distributed data set. Furthermore, anonymous post-course free-text feedback was sought to explore students’ experiences and perceptions of the course and recommendations for future improvement. Qualitative thematic analysis of the data was performed independently by two authors who employed an inductive approach and worked within a constructivist epistemology (12). Themes were combined and agreed upon collectively, with a selection of exemplar comments chosen to accentuate them (Table 1).
Ethical approval was not deemed necessary by our institutional ethical committee.
| Theme | Sub-Theme | Exemplar Comments |
|---|---|---|
| Knowledge Acquisition | Use of mini-teach tutorials | “The mini lectures at the end of each case was very helpful to consolidate knowledge” |
| “Mini lectures at end of scenario helpful in improving knowledge” | ||
| “It was really useful to talk through each topic after in the mini-lecture” | ||
| “Helpful ‘micro-teaching’ sessions for clinical knowledge” | ||
| “Liked the presentations after each station to cover the treatment of each case” | ||
| “Post scenario teaching was done well and helped cement the learning” | ||
| “Brief synopsis on disease afterward was appreciated” | ||
| “Post sim lectures were good for consolidating learning” | ||
| Use of pre-scenario tutorials | “Fluids talk was concise but really clear and helpful” | |
| “The fluids revision was particularly useful” | ||
| “Very useful having the intro lectures first as we then got more out of the sim” | ||
| “Revision of A-E + fluids before sim was useful” | ||
| “Interactive style of lectures” [was beneficial] | ||
| Simulation scenario content | “Scenarios were well tailored to our level of understanding and pertinent to paediatrics block” | |
| “Good overview of general paeds emergencies” | ||
| “Was useful to be made to think about differentials for each scenario” | ||
| “Covered broad range of scenarios” | ||
| “Realistic acute scenarios managed as they would be in reality” | ||
| Prescribing in paediatric patients | “Getting used to prescribing” [was beneficial] | |
| “Practicing medication + fluid prescribing” [was beneficial] | ||
| “Practice with prescribing/fluids/medications” [was beneficial] | ||
| “Some further cases where using a Kardex / actually having to write down prescriptions – as this is an area I don’t feel confident in” | ||
| Value of debriefing simulation scenarios | Length of debriefing sessions | “Lengthy feedback discussions- felt like the feedback portion could be less time consuming, so we would be able to do more simulation” |
| “Reduced debrief time would be better to make more time for clinical teaching”. | ||
| “Less time spent on debriefing and more time spent on scenarios”. | ||
| “Feedback sessions were constructive and not too long”. | ||
| Learning within debriefs | “Honest and constructive feedback from teachers” [was beneficial] | |
| “The teaching debriefs at the end of each scenario were very knowledgeable and helpful”. | ||
| “Good feedback from peers on how to improve”. | ||
| “Discussion as group/different perspectives helped clarify where improvements might be made in approaching management”. | ||
| “Non-judgemental feedback; allows constructive criticism of performance”. | ||
| “Reflecting on what went right and wrong in the scenario” [was beneficial] | ||
| “Really enjoyed the course and has really helped my learning & application of knowledge to clinical scenarios” | ||
| “Personalised feedback” [was beneficial] | ||
| “Lots of chances to ask questions” [was beneficial] | ||
| Appreciation of the importance of non-technical skills in clinical practice | Communication | “Practicing doing a phone-call handover- made it feel a bit more realistic and was a useful skill to hone” |
| “Good practice of SBAR” | ||
| “Communicating with parent, especially when you aren’t sure of exact plan / diagnosis” [was beneficial] | ||
| “Inclusion of a worried parent scenario very useful” | ||
| “Difficult communication station was very beneficial” | ||
| “Closing the loop- hadn’t been taught this before” [was beneficial] | ||
| Teamwork | “Focus on teamwork and non-technical skills” [was beneficial] | |
| Value of faculty expertise | - | “Good amount of teachers, varying expertise and teaching styles” |
| “Tutors were all knowledgeable and friendly- good teachers” | ||
| “Non-confrontational approach of tutors” | ||
| Value of repeated practice | - | “Repeat the simulation after having feedback and lecture” |
| “Part of practice is applying feedback on the next attempt- a second day or a smaller group would allow this” | ||
| “Would be very, very useful to have another go to actually learn from where you went wrong and improve on that” | ||
| Opportunities for exposure to pediatrics which is otherwise limited | - | “Rare opportunity to do this in the undergraduate curriculum”. |
| “Useful to get some practical paeds sim experience as we have never had it before”. |
4. Results
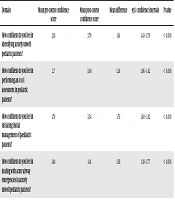
A total of 80 students attended the SimPLES course between November 2019 and March 2020. Unfortunately, due to the COVID-19 pandemic, further iterations of the course were temporarily suspended. All the students (100%) completed pre and post-course questionnaires to assess self-reported confidence across eleven domains (Table 2).
| Domain | Mean pre-course confidence score | Mean post-course confidence score | Mean difference | 95% confidence intervals | P value |
|---|---|---|---|---|---|
| How confident do you feel in identifying acutely unwell pediatric patients? | 2.18 | 3.79 | 1.61 | 1.43 – 1.79 | < 0.001 |
| How confident do you feel in performing an A to E assessment in pediatric patients? | 2.7 | 3.94 | 1.24 | 1.06 – 1.42 | < 0.001 |
| How confident do you feel in initiating initial management of paediatric patients? | 1.78 | 3.54 | 1.76 | 1.60 – 1.92 | < 0.001 |
| How confident do you feel in dealing with acute airway emergencies in acutely unwell pediatric patients? | 1.84 | 3.41 | 1.58 | 1.38 – 1.77 | < 0.001 |
| How confident do you feel in dealing with acute respiratory emergencies in acutely unwell pediatric patients? | 1.86 | 3.66 | 1.8 | 1.63 – 1.97 | < 0.001 |
| How confident do you feel in dealing with acute circulatory emergencies in acutely unwell pediatric patients? | 1.89 | 3.41 | 1.53 | 1.33 – 1.72 | < 0.001 |
| How confident do you feel in prescribing medications for acutely unwell pediatric patients? | 1.5 | 3.18 | 1.68 | 1.50 – 1.85 | < 0.001 |
| How confident do you feel in prescribing IV fluids for acutely unwell pediatric patients? | 2.1 | 3.94 | 1.84 | 1.64 – 2.04 | < 0.001 |
| How confident do you feel when escalating care to senior colleagues? | 3.11 | 4.04 | 0.93 | 0.73 – 1.12 | < 0.001 |
| How confident do you feel in communicating with parents of unwell pediatric patients? | 2.18 | 3.53 | 1.35 | 1.15 – 1.55 | < 0.001 |
| How confident do you feel in displaying effective non-technical skills during an acute emergency (e.g. communication, leadership, task delegation, situational awareness)? | 2.68 | 3.78 | 1.1 | 0.92 – 1.28 | < 0.001 |
Students reported statistically significant improvements in confidence across all eleven domains, with the largest increases seen in prescriptions of intravenous fluids and the management of respiratory emergencies (Table 2).
The comments in the post-course free-text questionnaire indicated that the vast majority of students have shared a positive and valuable learning experience. Thematic analysis of the data identified six core themes: knowledge acquisition, the value of debriefing simulation scenarios, appreciation of the importance of NTS in clinical practice, the value of faculty expertise, the value of repeated practice, and opportunities for exposure to pediatrics, which is otherwise limited (Table 1).
Data analysis demonstrated that the innovative post-scenario mini-tutorials were favorably viewed, allowing students to “consolidate knowledge” and “cement the learning”. Additionally, pre-scenario tutorials on pediatric A-E assessment and fluid prescriptions were well received. Data analysis also identified a “useful” and “helpful” focus on “practicing medication and fluid prescribing”, with these domains showing some of the largest increases in confidence following participation in the course (Table 2).
Interestingly, a significant minority of students reported a desire to participate in more scenarios, feeling that more learning would be achieved within the simulated environment than the following reflective discussions. This assumption may be more common in undergraduate immersive SBE due to undergraduates having little or no extra-simulated concrete experience to scaffold reflections during the debriefing process. Such perceptions were, however, overshadowed by numerous other students commenting that “discussion as a group” and “reflecting on what went right and wrong” were the strengths of the course and, by extension, a strength of immersive SBE.
5. Discussion
Despite the increasing prevalence of immersive SBE within the undergraduate curricula, there is limited evidence that currently justifies the associated costs and resources, especially in pediatrics (13). However, our study adds to the growing evidence base showing that immersive SBE leads to improved medical students’ self-reported confidence in managing pediatric emergency scenarios (5, 8) and enhanced student satisfaction (5, 8, 14, 15). A small number of studies have been expanded on this evidence. Drummond et al. reported that immersive SBE might lead to better knowledge retention among undergraduates learning pediatric emergencies, even at 12 months post-intervention when compared with traditional lecture-based education (16). One study described an improvement in summative objective structured clinical examination (OSCEs) scores for a group of students who had undergone an immersive SBE clerkship when compared to their predecessors who had not had the option of attending the clerkship (15). Dudas et al. report that incorporating immersive SBE within more comprehensive simulation-based initiatives could improve students’ clinical performance within their pediatric placements (13). However, due to the multiple SBE modalities, this study could not explicitly demonstrate causation between immersive SBE and clinical performance. Furthermore, conflicting reports suggest that immersive pediatric simulation, despite improved student satisfaction, has almost no effect on knowledge retention when compared to case-based discussions or learning via watching videos (17, 18). Overall, as suggested by Battista and Nestel, the discourse regarding whether or not immersive SBE ‘works’ has now moved on towards discussions about the most effective and meaningful methods to employ its use within medical education (2).
We also demonstrate the value of incorporating mini-tutorials within an immersive SBE course design to consolidate learning and knowledge acquisition within an undergraduate cohort, which deviates from traditional practice within immersive SBE. If participants become fixated on discussing particular technical aspects of a scenario, faculty can defer this to the mini-tutorial, thereby allowing more profound exploration and reflective practice of the experience itself within the debrief. Such innovations may be even more significant when running immersive SBE courses related to specialized topics with limited clinical exposure. In our experience of such cases, students often perceive the technical aspects of each case with more importance than in clinical scenarios with which they are more familiar. It is necessary to conduct further qualitative research that employs more robust methods such as semi-structured interviews or focus groups to explore and quantify these concepts.
There are several significant limitations to this study. Firstly, our evaluation is based on students’ self-reported confidence. Self-reported confidence does not equate to the observed measures of competence and is notoriously inaccurate in both undergraduate and postgraduate medical populations (19, 20). Further research is needed in the setting of undergraduate pediatric immersive SBE to assess if self-reported confidence translates to improved clinical performance. Secondly, our study is limited to three sites within the west of Scotland and therefore may not be generalizable to other centers providing undergraduate pediatric medical education. Thirdly, our evaluation is limited to one academic year, so selection bias may distort our results. Fourthly, our evaluation occurred immediately following the delivery of the SimPLES course. Longitudinal research would facilitate a more reliable appreciation of the longevity of confidence improvements, on which we are currently unable to comment. Fifthly, while free-text comments can provide some insight, alternative qualitative research methods such as semi-structured interviews and focus groups may provide more robust data. Finally, our course is uni-professional, both in terms of the candidates as well as faculty. We are therefore unable to comment on how skills would translate to emergency scenarios in which an inter-professional team was working together.
5.1. Conclusion
Despite these limitations, our study has demonstrated that, although not a replacement for real clinical exposure, immersive SBE is a viable and effective method of education delivery within the undergraduate pediatric curriculum. Our study adds to the growing evidence-base showing that SBE improves self-reported confidence of medical students in assessing and managing acutely unwell pediatric patients and can highlight and emphasize the importance of NTS in the clinical workplace. Furthermore, incorporating mini-tutorials within an immersive simulation course design in an undergraduate setting is helpful for medical students. Further research is required to assess whether these changes can be replicated on a larger scale and whether improvements in medical students’ self-reported confidence can be translated into improved observed clinical competence.